Breast Augmentation Special Offer
Improve Your Confidence and Enhance Your Silhouette with Breast Augmentation in Bellevue, WA
David Stephens, MD Plastic Surgery | Aesthetics
Voted Best Cosmetic Surgeon for 10 Consecutive Years.
*Offer Expires February 28, 2026
Featuring Motiva® Breast Implants A New Gold Standard in Breast Implants
Dr. David Stephens is one of the first plastic surgeons in the Northwest to offer Motiva® breast implants. With unmatched safety and patient satisfaction, Motiva® breast implants are only sold to board-certified plastic surgeons, ensuring device integrity and optimal results.
Achieve your aesthetic goals with some of the most trusted breast implants in the industry. Claim $500 off your breast augmentation with Dr. Stephens today!
*Offer Expires February 28, 2026
Breast Augmentation with Motiva® Breast Implants
Breast augmentation is a surgical procedure designed to enhance the shape, volume, and appearance of the breasts.
Dr. Stephens uses Motiva® implants for breast augmentation because of their natural look, safety, and advanced technology.
Proven Results:
- 97% patient satisfaction
- 99% surgeon satisfaction
- Only 0.5% capsular contracture rate
- Only 0.6% rupture rate (vs. 7–8% with older implants)
- No reported cases of BIA-ALCL
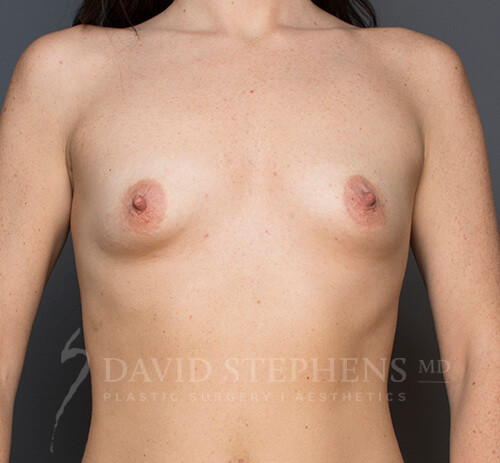
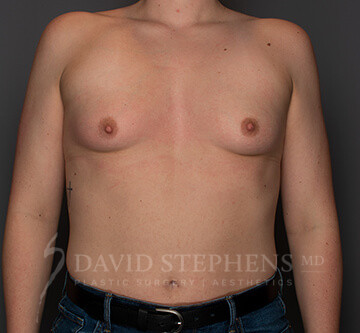
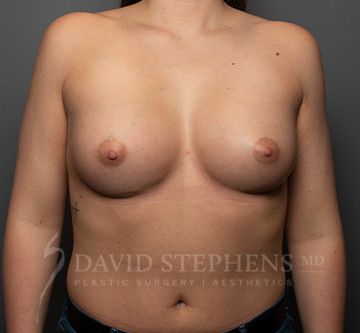
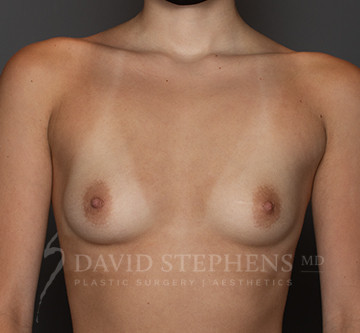
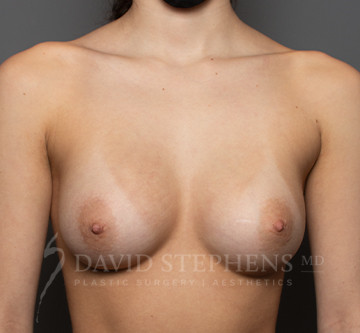
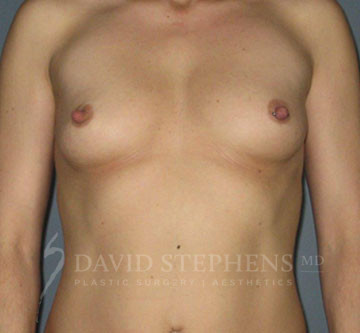
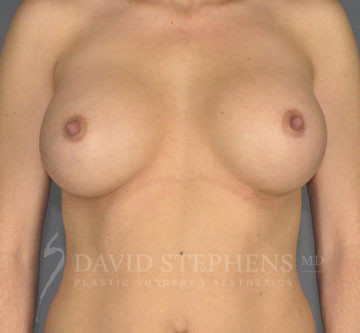
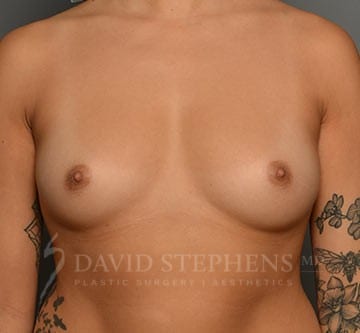
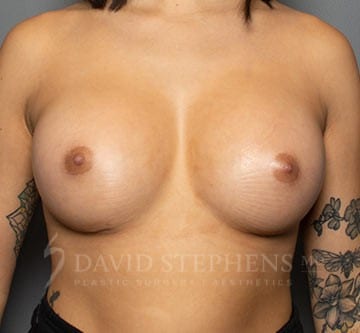
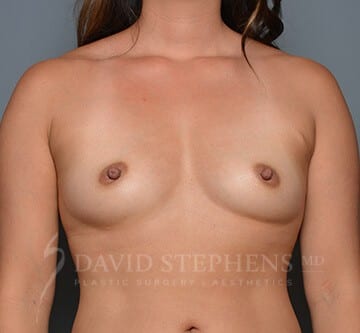
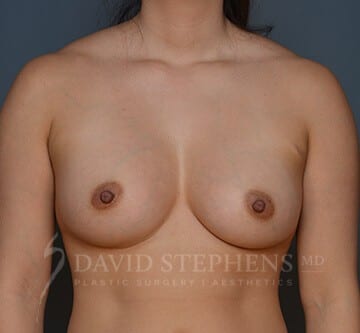
Before & After
Before-and-after patient photos are available upon Consultation.
Financing
12 months 0% APR Financing.
Low Monthly Payments!
“Dr. Stephens and his team were AMAZING! They truly care for your needs and the outcome was perfect! I couldn’t have gotten a better surgeon for my breast augmentation! They were very detailed, always made sure that I knew and understood everything I was going to go through.”
“Dr. Stephens and his staff have been amazing throughout the process of my breast augmentation. It is obvious how good the dr is at what he does during the consultation. He doesn’t just give you what you want, but instead informs you of what will look best. As someone who works in the medical field, I often have high expectations and can sometimes be overly critical. I have nothing to criticize. The entire experience has been perfect. My breast look better than I even expected.”

The Four Pillars of Motiva® Technology
At Stephens Plastic Surgery in Bellevue, Seattle, we are proud to offer Embrace™, an advanced, minimally invasive facial rejuvenation treatment that combines FaceTite™ and Morpheus8™ technologies.
1. SmoothSilk® Surface
Ultra-fine 4-micron surface mimics natural tissue, reducing inflammation and lowering the risk of capsular contracture.
2. Monobloc® Construction
The implant shell, gel, and patch are made as one structure for durability, softness, and less rippling — plus smaller incisions. Patients also enjoy more natural movement and feel compared to other silicone implants.
3. BlueSeal® Barrier
A built-in safety feature that ensures shell integrity during the manufacturing process and beyond, with easy visual inspection.
4. 6th-Generation Gel
A high-strength cohesive gel that feels soft, natural, and moves like real breast tissue. This advanced silicone gel implant creates significantly less internal and external friction, providing a natural feel that patients love.
Warranty: During your consultation, we will provide information about the Motiva® Health Program and Motiva® Health Program Plus.
*Offer Expires February 28, 2026

Enhance Your Silhouette with Motiva® Reserve Your Spot Now!
Get $500 off your breast augmentation and experience the next generation in safety, softness, and natural beauty.
*Offer Expires February 28, 2026

Why Choose David Stephens, MD Plastic Surgery | Aesthetics?
Dr. David Stephens is one of the Northwest’s premier breast surgeons, known for his artistic sensibility, meticulous care, and natural-looking results. Voted “Top Cosmetic Doctor” by 425 Magazine for 10+ years, he’s trusted by thousands of patients—including medical professionals and celebrities—locally, nationally, and worldwide.
At your consultation, you’ll experience the advanced VECTRA® 3D imaging system, giving you a realistic preview of your results. Dr. Stephens has a relaxed but thorough style, taking the time to understand your goals and design a personalized surgical plan just for you and your goals.
All procedures are performed in our AAAASF-accredited surgery suite under the guidance of our board-certified anesthesiologist and a highly experienced surgical team that is attentive to every detail, ensuring your safety, privacy, and comfort.
Choose Dr. Stephens for timeless, elegant breast augmentation results—backed by decades of experience and a reputation for excellence.
*Offer Expires February 28, 2026
Patient Testimonials
“I wish I could give this more than five stars! I met with several surgeons in the area before deciding on Dr. Stephens for my breast augmentation and let me tell you, I am so happy I did. I have always felt self conscious about my breast size and thanks to Dr. Stephens, I have a new-found confidence. The results are beautiful and exceeded all my expectations. I had a lot of anxiety about surgery and the entire staff, Dr. Stephens and Dr. Brandford made me feel right at home.”
I would definitely recommend Dr. Stephens to my family and friends. There is a reason he is the best of the best!
“Dr. Stephens and his team were AMAZING! They truly care for your needs and the outcome was perfect! I couldn’t have gotten a better surgeon for my breast augmentation! They were very detailed, always made sure that I knew and understood everything I was going to go through.”
“From start to finish, Dr. David Stephens and his staff have been amazing. Karina at the front desk is always so inviting and on top of it. Nurse Rosemary is very explanatory and caring. Lori the office manager is organized and easy to talk to. I cannot express how grateful I am with my breast augmentation results, and how amazing Dr. Stephens’ work is! Thank you to all the staff for making this such a positive experience.”
What Our Patients Are Saying
FAQs
- What kind of anesthesia will be used for my surgery?
- Is there a minimum recommended age for breast augmentation?
- Do I need to replace my implants every 10 years? How long do breast implants last? When do you recommend MRI and ultrasound studies for my implants? When will I need to replace my implants?
- Do breast implants include a warranty? For failure or disruption of the implant shell? For capsular contracture?
- Do breast implants interfere with mammography?
- What are the immediate risks associated with breast augmentation?
- What is capsular contracture? What can I do to avoid capsular contracture?
- Who are the best candidates for breast augmentation?
- What are the long-term risks of breast implants that I should be aware of?
- Which implants do you currently recommend? Silicone gel versus saline? Round versus teardrop-shaped? Textured versus smooth?
- What is ALCL? BIA-ALCL? What should I do if I see my breasts become larger after my procedure?
- How do I choose the best size breast implant for me?
- Is there a risk of breast cancer after breast implants?
- Will a broken or “ruptured” implant make me sick? How will I know if it is broken?
- Should I get regular mammograms following my breast augmentation?
- How much pain should I expect after my breast implant surgery?
- How soon will I be able to go to work?
- How soon can I exercise after breast augmentation?
- When can I have sex?
- How soon may I lift my child?
- How long will it take for my breasts to look “natural”?
- When can I shower?
- When are my appointments following my breast implant surgery?
- When can I sunbathe?
- When can I drink alcohol? When can I smoke?
- What type of bra should I wear following my surgery?
- Do I massage my breasts following my procedure? What about stretching?
- What about if one breast looks different from the other following the procedure?
- What if there are other things that I didn’t expect?
Breast Augmentation Frequently Asked Questions
-
What kind of anesthesia will be used for my surgery?Breast augmentation is performed using light, short-acting general anesthesia, which is administered by our anesthesiologist. Dr. Stephens will place a nerve block around the breast during your procedure as well.
-
Is there a minimum recommended age for breast augmentation?Breast augmentation with saline implants can be performed for patients 18 years and older; however, silicone implants are FDA-approved only for patients aged 22 and older. Silicone implants may be used in women under 22 years of age, but it is considered “off-label” and the manufacturer’s warranty is null and void, so this is not recommended.
-
Do I need to replace my implants every 10 years? How long do breast implants last? When do you recommend MRI and ultrasound studies for my implants? When will I need to replace my implants?It is a common misconception that you should have your implants replaced every 10 years, as studies show that less than 10% of breast implants have been disrupted from implant shell failure, or “ruptured.” So why replace the 90% that are still perfectly good?! There is no particular time an implant will fail; it’s only a statistical estimate, but we think implants fail at around 1% per year or less, increasing as they get older. We don’t have good data after 10 years, as the FDA does not require studies longer than 10 years.
We highly recommend an MRI or high-definition ultrasound at five years, and every three years thereafter. Because of the 10-year warranty on many implants, be sure to have a study done before then if you haven’t already. It is highly likely that your implants will need to be replaced in your lifetime, so it is important to monitor them carefully. Keep your manufacturer’s warranty and your implant information in your files for reference, as the warranty is provided specifically by your manufacturer.
-
Do breast implants include a warranty? For failure or disruption of the implant shell? For capsular contracture?Breast implant warranties are provided by manufacturers and typically cover the cost of a replacement implant and a portion of the replacement surgical costs for implant failure within the first 10 years. The Sientra® warranty is considered the best standard warranty in the industry for both implant failure and capsular contracture. The Motiva® Health Program Plus costs $250 and is highly recommended. Other manufacturers also provide a limited warranty for capsular contracture. Dr. Stephens’ office will provide copies of these warranties upon request and discuss their details during your consultation. Warranty information is also available on the manufacturer’s websites. Warranties may change at any time, so it is best to keep yours on file or call the office if you have questions. There are no warranties for other re-operative procedures; however, Dr. Stephens offers a reduced fee for this within the first year after your surgery, depending on the cause and situation.
-
Do breast implants interfere with mammography?Yes, to a variable degree, but this hasn’t increased the risk of breast cancer nor the risk of delayed diagnosis of cancer in clinical studies. Breast implants in the submuscular or “dual plane” interfere much less with mammography than above-muscle implants. During your mammogram, your technician will utilize a special view called the “Eklund View” to bring the implant behind the breast tissue, thereby minimizing the areas that are not visible. Newer digital and 3D mammograms are significantly more effective as a screening tool. Newer high-definition ultrasound systems are also much more sensitive in questionable areas as an adjunct to mammograms. MRI is a very sensitive way to assess for early breast cancer, but it has more false positives, where they see a suspicious area that turns out to be normal with biopsy.
-
What are the immediate risks associated with breast augmentation?As with any surgical procedure, there are some risks involved with breast augmentation. We take every precaution necessary to make sure each patient is in a safe environment. While complications are uncommon, they can include:
- Unfavorable scarring: We rarely see poor scarring after breast augmentation, and this is typically genetic and skin tone-based, not because of the surgical incision per se. We strongly recommend scar care with Biocorneum® and pigment lighteners for all our patients and follow-up care for the first year to assess how the scar is doing, among other things.
- Reactions to anesthesia: This is very rare; there is a rare genetic mutation to general anesthetics that most people inherit from their relatives, so this history is critical to know, but otherwise, the risk of a catastrophic event from general anesthesia is actually less than from sedation (a well-known secret in the industry).
- Bleeding: Hematomas, or bleeding in the breast pocket, requiring exploratory surgery, are extremely rare in breast augmentation. However, it is important to limit impact activities in the first few weeks after your procedure to reduce your risk. Hematomas have rarely occurred in our practice, but the ones that did happen were two or so after the patient felt so good that they engaged in too much activity. So limit your activity to what we recommend for you. We will provide a list of instructions following your surgery to ensure the best possible results.
- Infection: This is very uncommon; we utilize a specific, hospital-grade skin preparation protocol used for orthopedic joint replacements and cardiac surgery, which we will teach you about in your pre-op appointment. We think that this is also one of the reasons that we have an extremely low rate of capsular contracture.
- Changes in breast skin or nipple sensation: While there is usually a temporary reduction and occasionally a temporary increase in sensitivity following breast augmentation, the risk of permanent loss of sensation to the breast or nipple is extremely rare. There is a higher risk if very large implants are used, but even then, the risk of permanent loss of sensation is rare. As the sensation recovers, it often returns with shooting or minor pain for a few weeks. On rare occasions, the return of sensation may take months to return, so patience is key.
-
What is capsular contracture? What can I do to avoid capsular contracture?Capsular contracture occurs when the normal response of the scar tissue surrounding the breast implant becomes thicker and tighter, causing the implant to feel harder, move upwards on the chest, become more round and ball-like, and shrink. The breast is slightly firm in mild cases and becomes increasingly firm with greater breast distortion, progressing to extremely hard in more severe cases. The recommended treatment is revision surgery with complete removal of the capsular scar tissue and existing implant, replacing the implant with a new one for more severe contractures. Dr. Stephens may provide a prescription for a medication for mild breast firmness if this happens. However, it is often the case that one breast may just be a bit firmer due to one breast pocket being tighter than the other, which evens out over time.
Recently, strong evidence has emerged that capsular contracture is a response to normal skin bacteria contaminating the implant surface. The bacteria send a biological signal to the capsular tissue to produce the excessive scar response. The risk of contracture ranges from 10 to 15 percent in some earlier studies and has been twice to three times this risk when the implant is placed above the muscle. Happily, with the current use of special pocket irrigation with antibiotics, ultra-sterile techniques, and skin preparation with special antiseptics, the risk is now between 1 and 2 percent over 10 years.
Dr. Stephens uses these protocols, as well as the Keller Funnel®, which protects the implant from ever touching the skin. This has been shown to reduce the risk of capsular contracture to less than 1% in his practice, regardless of incision placement.Dr. Stephens highly recommends that his patients take pre-dental antibiotics before any dental procedures or teeth cleaning. There is clear evidence that capsular contracture can be caused by mouth bacteria during these activities, and we have seen this from some of our consultations as well.
-
Who are the best candidates for breast augmentation?Women with smaller breasts may not feel feminine or confident in their appearance. They want their breasts to be proportionate to the rest of their body. Other women may have lost all of their breast tissue in breastfeeding and the rapid weight gain and loss of pregnancy. There are women whose breasts are misshapen, asymmetrical, or have deformities that are only correctable with breast surgery and implants. Of course, patients must be in good health, understand the long-term care, and agree to be proactive in the care of their implants.
-
What are the long-term risks of breast implants that I should be aware of?The positive effects of breast implants are not to be minimized. Women often experience heightened self-esteem and pure joy when they look and feel more feminine and confident in and out of their clothes. There are multiple studies that show that women have a greater than 95% extremely satisfied rate following breast augmentation.
It is important to recognize that breast augmentation is not a “one-and-done” procedure. While it is rare to get an infection or breast pocket hematoma, capsular contracture can occur, requiring surgery in 1 to 2% of patients with good practices. Implant failure requires implant replacement surgery in 10% of patients after 10 years. Implants can move out of position and require reinforcing procedures, such as repairs, meshes, or other materials. Implants can thin the breast tissue over time, particularly if placed above the muscle. Often, a painful breast is the result of the implant moving towards the armpit and pressing on nerves along the side of the chest or because of capsular contracture.
It is important to recognize that a ruptured silicone implant may be completely silent, which is why we recommend periodic MRI or high-resolution ultrasound of the breasts to assess for rupture. With the newer highly cohesive implants, the gel material may completely stay within the broken shell, but the broken barrier will result in a gradual seepage or very minute amounts of silicone. This is not a risk of disease, but it may accumulate in lymph nodes if left alone for years, so MRI is important with silicone implants. Saline implants will just leak sterile water, and the implant will go flat, with an obvious change in size and shape.
-
Which implants do you currently recommend? Silicone gel versus saline? Round versus teardrop-shaped? Textured versus smooth?Dr. Stephens currently recommends Motiva SmoothSilk® due to its low risk of capsular contracture and rupture. He may recommend smooth-round silicone implants from another manufacturer in certain situations. With experience using various types of breast implants through the years, he finds that Motiva SmoothSilk® provides the best combination of natural softness, feel, and shape with the least amount of complications.
Saline breast implants are not as soft and pliable nor as natural-looking as the newest cohesive silicone gel implants. Saline-filled implants may be a good alternative for a woman who does not like the prospect of having imaging studies done, such as MRI studies. It is also an option for young women who have good breast shape and tissue. Standard saline implants are less expensive than silicone implants. However, more than 90% of our patients choose the newest cohesive silicone implants.
If you have the Allergan™ Biocell breast implant, you should see a plastic surgeon and review your options for removal. There is new evidence that the macro-textured Allergan™ implant has a significantly higher risk of a type of breast lymphoma called BIA-ALCL. They are found in the teardrop-shaped “gummy bear” silicone and textured round implants. The risk of ALCL with the Allergan™ textured implant is somewhere between one in 3,000 (seen in Australia) and one in 30,000 women. It is treatable and curable when caught early with the removal of the breast capsular tissue. It presents with an enlarging fluid-filled breast.
-
What is ALCL? BIA-ALCL? What should I do if I see my breasts become larger after my procedure?Breast Implant-Associated Anaplastic Large Cell Lymphoma (BIA-ALCL) is a rare type of lymphoma. It has recently been increasingly associated with Allergan™ Biocell macro-textured implants and is associated with a rapidly enlarging fluid collection called a seroma that typically occurs several years following breast augmentation. The risk of ALCL in the U.S. is about one in 3,000 women. The Allergan™ macro-textured implant is a type of polyurethane-coated implant (not FDA-approved for use in the U.S.) that is most commonly associated with BIA-ALCL, though it is rare in other textured breast implants. ALCL has been associated with other types of implants, including orthopedic prosthetics.
If you experience an enlarging breast, it is important to see Dr. Stephens or your plastic surgeon immediately to be examined. If ALCL is a consideration, you will be referred to a breast radiologist for assessment and further investigations. If caught early, BIA-ALCL is treatable and curable with the removal of the implant and complete removal of the breast implant capsule (total capsulectomy). However, if ignored, ALCL can be deadly.
-
How do I choose the best size breast implant for me?We like to say that there is a perfect fit of a breast implant for your breasts. It is much like the fit your hand has in the ideal glove or how your foot should fit nicely inside of your shoe. There is the “base width diameter” (the “footprint,” or shadow) that your breast has on your chest. If the implant width exceeds this diameter by too much, it will be sitting in your armpit and under your collarbone. If it is too narrow, it won’t fill out your breasts enough to give them shape, and there will also be too much distance between the breasts and a loss of cleavage. As breast implants of any given profile get larger, they get wider, and as they get smaller, they get narrower; a moderate profile implant that is 400cc is wider but doesn’t have much difference in profile or projection than a moderate profile 300cc implant.
The “perfect fit.” We like to call it the “Goldilocks Syndrome:” not too big, not too small, but just right! A breast implant that is sized carefully will look good and natural. Once the base width diameter is established, there are considerations of the type of profile or projection to use based on the woman’s body shape, height, torso, breast shape, breast firmness, and her realistic desires and expectations. And the VECTRA® 3D Imaging System will simulate how your breast changes with different implants.
-
Is there a risk of breast cancer after breast implants?Long-term studies of breast implants show that there is no higher risk of breast cancer or any other cancer in women with breast implants than in women without implants. They also show that the cancers are not detected later, nor are they more aggressive.
-
Will a broken or “ruptured” implant make me sick? How will I know if it is broken?A broken saline implant will deflate within a period of days or weeks, and the salt water just dissipates into your tissues as you notice the breast deflating and flattening. It is not an emergency to get it fixed, but waiting too long will cause the capsular tissue around the implant to collapse and may require additional surgical procedures at the time to reshape the capsular tissue that may collapse. Our bodies are partially made of saline, so it does not pose any health risks.
A broken, or “ruptured,” silicone gel implant may silently leak from the outer shell into the breast pocket, but it rarely goes into the breast tissues unless it is a very old implant, it has been leaking for a very long time, or there has been some trauma. We call this a silent rupture, and we recommend periodic MRI or high-definition ultrasound to assess implant integrity. The silicone gel may leak from the implant in microscopic or nanoscopic amounts over time, making it important to replace a broken gel implant; however, there is no evidence that the silicone gel causes any illness or disease. It is difficult to impossible to diagnose a broken implant by examination, but a change in breast shape or capsular contracture may be a clue to consider a “ruptured” implant. It may not be seen on mammography but can usually be identified by high-resolution ultrasound and, particularly, MRI.
The newest generation of highly cohesive silicone gel implants, particularly from Motiva® and Sientra®, is soft and well-attached to itself and to the implant shell. The gel has been shown not to escape the implant shell when it breaks. Silicone gel implants do not cause any implant-related illness when the shell breaks.
-
Should I get regular mammograms following my breast augmentation?Mammograms are recommended to screen for breast cancer after breast augmentation. The technician should ask you if you have implants and will do special techniques to bring the breast tissue in front of the implants. Radiologists may recommend additional studies depending on the breast tissue density and family history of breast cancer. There are different recommendations for when to start getting mammograms based on family and personal history, but in general, the consensus among plastic surgeons is that mammograms should be done by age 40, prior to surgery, without specific risk factors. It is important to provide a thorough history of any breast conditions, biopsies, and family history of the risk of breast cancer.
-
How much pain should I expect after my breast implant surgery?While we do not subscribe to the “24-hour rapid recovery” philosophy due to concerns of confirmation bias, we see that our patients experience pressure in their chest or a feeling that they are breastfeeding and the milk is coming. We have developed a combination of medicines to help with this, including a combination of acetaminophen, a muscle relaxant, providing specific medications and techniques in surgery, and early activity within reason that includes early stretching and gently fitting garments. We provide narcotic pain medicines for breakthrough pain that can occur at nighttime in the first week, but many patients don’t find a need for this. Ibuprofen (Advil® or MOTRIN®) or naproxen (Aleve®) can be used after five days and work well as pain relievers.
-
How soon will I be able to go to work?This depends on the type of work you do. Most women can return to non-physical work in a week, possibly sooner, following their implant surgery. If you do very physical work, you may need to plan or return to light duty for several weeks after the procedure. We recommend being very careful of extreme activity for 8 to 12 weeks following implant surgery, as this may cause the implants to slip out of the pocket and bottom out or move into the armpits.
-
How soon can I exercise after breast augmentation?We recommend doing light activity immediately after your breast augmentation procedure, including walking and stretching. Avoid any exercise that could raise your blood pressure or pulse rate, and avoid extreme positions for the first two to three weeks to reduce the risk of bleeding. You should be able to begin light cardio exercise in three to four weeks as long as you keep your effort around 50 to 60 percent of heavy effort, and it is non-impact. This may include an elliptical or stationary bike, or walking on a treadmill. You may increase your walking effort over the first month to six weeks and even begin light running at this time. It is important to avoid heavy impact exercise for eight weeks and not work your pectoral muscles for three months in order to allow the supportive scar tissue capsule to mature. This is the only thing supporting your implants, so it is important to be careful with it.
-
When can I have sex?Believe it or not, we get asked this question a lot! Sexual activity, if done gently, may begin as soon as you are comfortable, as long as you keep your pulse rate within reason and avoid putting stress on your chest.
-
How soon may I lift my child?It is important to use your back and legs when lifting a child or infant, and to keep your arms close to minimize the risk of them getting outstretched. If you are careful, you may lift a cooperative and quiet child up to 35 pounds. Do not try to bend too far or stretch to pick up a child, such as from a car sea,t where you are overextended, or from a playpen, where you have to stoop a lot. Use your core to carry and lift your child and keep your arms quiet.
-
How long will it take for my breasts to look “natural”?Your breasts will typically look high in the first several weeks to even months following your procedure, depending on their projection and the tightness of your tissues. This is because although your breast implants may be the proper size, the upper part of the breast implant pocket below the muscle in the dual plane procedure is much looser than the lower part of the implant pocket, where the tissue is tighter, so the implant needs to settle and stretch out the lower area. The breasts are also swollen, and the implants are tightly “squished” by your tissues, so this takes time to relax and for the shape to develop. It is like a poorly focused picture that becomes increasingly sharp over time. Overall, it takes six months to a full year to see the final result, which is why we like to see you for a one-year follow-up.
-
When can I shower?You can shower in 48 hours following your procedure. Take off and replace the gauze dressings, but do not remove the flesh-colored tapes on the incisions. We do not recommend taking a bath in the first few weeks following your surgery.
-
When are my appointments following my breast implant surgery?We typically see you one within a week or so following your procedure, followed by a visit at one to two weeks, followed by two weeks to one month, three months, six months, and one year. We are available to see you if there are any problems following your procedure at any time. There are no drains in breast augmentation surgery, but the incisions need to be assessed and any sutures removed, if necessary.
We are available to see all and any of our breast implant patients indefinitely at no charge after their breast augmentation if they have any questions or concerns, and we are available to answer any questions at any time following your breast implant procedure.
-
When can I sunbathe?You may go in the sun immediately after your procedure, as long as you keep your breasts covered with sun-resistant clothing and beachwear, and use a good sunscreen applied frequently. Keep the incision out of the sun or UV rays for a year, or more if you have a darker skin type. We recommend Biocorneum®, which contains sunscreen for incision care, but be sure to protect the incision from direct sunlight.
-
When can I drink alcohol? When can I smoke?As long as you are not taking narcotics, you may have a small amount of alcohol after a week. It can run a higher risk of bleeding and should be avoided initially.
Smoking affects healing. There is no consensus regarding the timing of stopping smoking, but suffice it to say that it does affect the body’s healing ability. The effect is not as profound in a small breast implant incision, but as a precaution, heavy smoking should be avoided for several weeks, and any smoking will theoretically slow down wound healing. Smoking prior to anesthesia will affect the irritability of the lungs and respiratory system and should be avoided for one to two weeks prior to your surgery to reduce this effect.
-
What type of bra should I wear following my surgery?We provide a post-surgical bra for your breast augmentation surgery that opens to the front to allow for easy access to your incisions. In addition, we provide a band above your breasts to hold them in position and to provide gentle resistance to the normal tendency for the implants to rise up towards the neck. As soon as you are comfortable, you may go into any bra as long as it doesn’t push up the breast implants. Underwire bras may press against the breast fold and may be uncomfortable, and some may push up, so this is not recommended if they do. A sports bra with a nice cup often works well after the first few weeks. We do not recommend purchasing a lot of expensive bras for three months or until the breast implants have settled and the swelling has diminished.
-
Do I massage my breasts following my procedure? What about stretching?We do not recommend traditional breast massage as defined by moving the implants all over, as it has not been shown to have any benefit in reducing the risk of capsular contracture (see capsular contracture information above). We recommend simple pocket-stretching procedures to expand the lower part of the breast implant pocket, allowing the implant to settle and relax the lower portion between the nipple and the breast fold below.
Movement and stretching of the chest and arms have been shown to speed up the recovery and reduce pain and tightness following breast surgery. Lack of movement causes muscle stiffness, so it stands to reason that gentle movement and stretching will speed up recovery. We recommend gentle stretching exercises for the chest muscles using arm movements to open the chest and shoulder girdle. We will show you these in the first week or two following your procedure. They are very effective in reducing pain and speeding up the recovery phase.
-
What about if one breast looks different from the other following the procedure?It is totally normal for the breasts to look different in the first weeks to even months following the procedure. Dr. Stephens points out to his patients that no two breasts are exactly alike, and the swelling from the procedure will often accentuate these differences, which will settle and become more similar over time. Sometimes, the smaller breast may paradoxically look larger following the procedure until time allows the skin and tissue to relax around the implant.
-
What if there are other things that I didn’t expect?If there is a significant difference between the breasts in the first few weeks after the procedure, especially over a short period of time, and this is accompanied by pain, this may be bleeding in the breast pocket, causing a hematoma that requires surgical exploration to stop the bleeding. Unusually, increased pain, high fevers, redness, or any discharge from the incision should be assessed by the office. A low-grade fever following anesthesia is normal. Any unusual or unanticipated symptoms should be reported to the office. We would rather hear from you than have something get worse that could have been addressed in a timely manner.